Identifying Social Determinants of Health
70% of health outcomes are determined by factors that take place outside hospital walls, and are often referred to as social determinants of health (SDOH). Understanding the various kinds of SDOH that exist and the impact they can have on a patient's well being has an important role in a patient’s care journey. In some cases, it may be difficult to identify social determinants of health but technology is helping uncover data that is useful in identifying SDOH both quickly and more easily.
What are social determinants of health?
Social determinants of health are conditions in the places where people live, learn, work, and play that affect a wide range of health outcomes. This includes both economic and social factors, such as education, income, or race. The availability of resources in the community and one’s access to care contributes to one’s overall health.
What are the 5 key areas of SDOH?
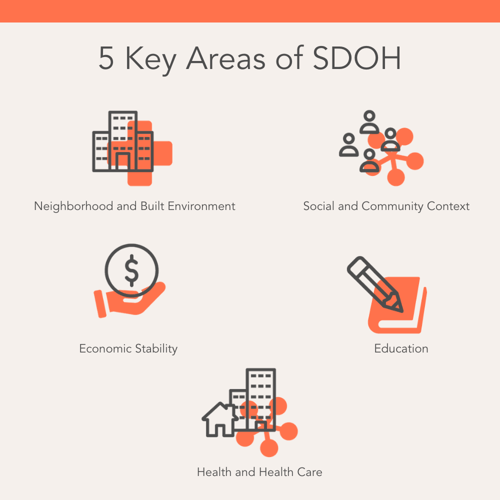
According to Healthy People 2020, there are five key areas of SDOH. These areas include neighborhood and built environment, social and community context, economic stability, education, and health and health care. Each of these areas include numerous factors, such as health literacy, employment, food insecurity, housing, or culture, that are examples of social determinants of health.
How technology helps identify SDOH
Technology such as artificial intelligence (AI), machine learning (ML), and natural language processing (NLP) can help health systems identify, prioritize, and address a patient’s social vulnerabilities. Using AI, ML and NLP to analyze electronic medical records, the notes of a physician, case manager, and social worker can be read to identify social determinants of health that might otherwise be missed. AI extracts valuable pieces of information that clinicians can use to make decisions on how to allocate resources to those who need it most. Being able to identify SDOH easily and more efficiently is important because it allows social determinants of health to be addressed and also helps improve hospital outcomes. One study found that SDOH contributed to more than 50% of hospital readmissions. Pieces Predict’s Social Determinants of Health module aids hospitals in combating the high costs and other issues associated with hospital over-utilization and excess lengths of stay.
Sometimes it can be difficult to screen for SDOH. Some patients may be unwilling to answer questions verbally about social or economic issues that they may be facing. This is where technology comes in to help. With the help of artificial intelligence (AI), chatbots can be used to ask questions to patients to screen for SDOH. This AI tool can scale to be used to serve more people than traditional teams alone, reducing manual effort. Being able to identify social determinants of health means that physicians and care managers are able to begin addressing these issues by connecting individuals with community resources.
Connecting to community resources
Once vulnerabilities are identified, care managers are now able to understand what a patient’s needs are beyond hospital walls. Identifying SDOH, often uncovers that a patient needs assistance from a food pantry, clothing shelter, or mental health professional. Through the use of Pieces Connect, a cloud based case management and referral directory, doctors and hospital case managers are able to send electronic referrals for their patient to resources in the community. With closed loop referrals they are also able to see the status of the referral, giving them visibility into whether their patient received the additional assistance needed. Pieces Connect’s robust and up-to-date referral directory offers information on a wide range of resources in the community. Connecting to these community resources can have a positive impact on a patient’s health outcomes and may even reduce their chance for readmission in the future.
Ready to learn more? Contact us today!

