Artificial Intelligence & the Restoration of the Medical SOAP Note

SOAP notes, or progress notes, are the part of a patient's medical record where healthcare professionals record a concise yet comprehensive summary of the patient's clinical status during the course of a hospitalization or medical encounter. A well written clinical SOAP note may arguably be one of the most effective, and valuable, forms of communication in medicine. Well-written ones can even be appreciated for their elegance, and convey in their concision, accuracy, and comprehensiveness everything a fellow provider must know to help their patient. Many clinical practitioners would now agree, however, properly constructed SOAP notes are becoming rarer. Many features of our modern medical environment get in the way of constructing the ideal note. We find that notes are now cluttered with information required for billing, legal, administrative and even research purposes, misfigured by auto-populated data, bloated by copy-and-pasted text, and riddled with data and sentence fragments. Modern clinical notes have been stretched and distorted so as to have become almost unrecognizable to their classical roots in medicine.
As I observe the progress of language AI systems, at Pieces and elsewhere, in which emerging software can both “interpret," "comprehend”, and “explain” a clinical scenario, I am convinced that healthcare providers – and patients – will one day soon have AI systems that will restore the SOAP note to its central role in medical care and communication. The implication for the quality, safety and the joy of healthcare delivery could well be profound. We may even approach a machine-generated note that, with human supervision, comes close to the original vision of its famed inventor, Dr. Lawrence Weed.
In this blog series, I am going to talk about the history of the SOAP note and our work at Pieces to automate their construction.
Part 1: Ode to the SOAP note
The SOAP note was introduced in the 1950s by Dr. Lawrence Weed, as a device to frame and formalize clinical reasoning within the medical record. (Wright et al. 2014) I’d encourage you to read Dr. Weed’s seminal 1968 paper in the New England Medical Journal “Medical Records that Guide and Teach” to see how his vision for the medical record all comes together. (Weed 1968).
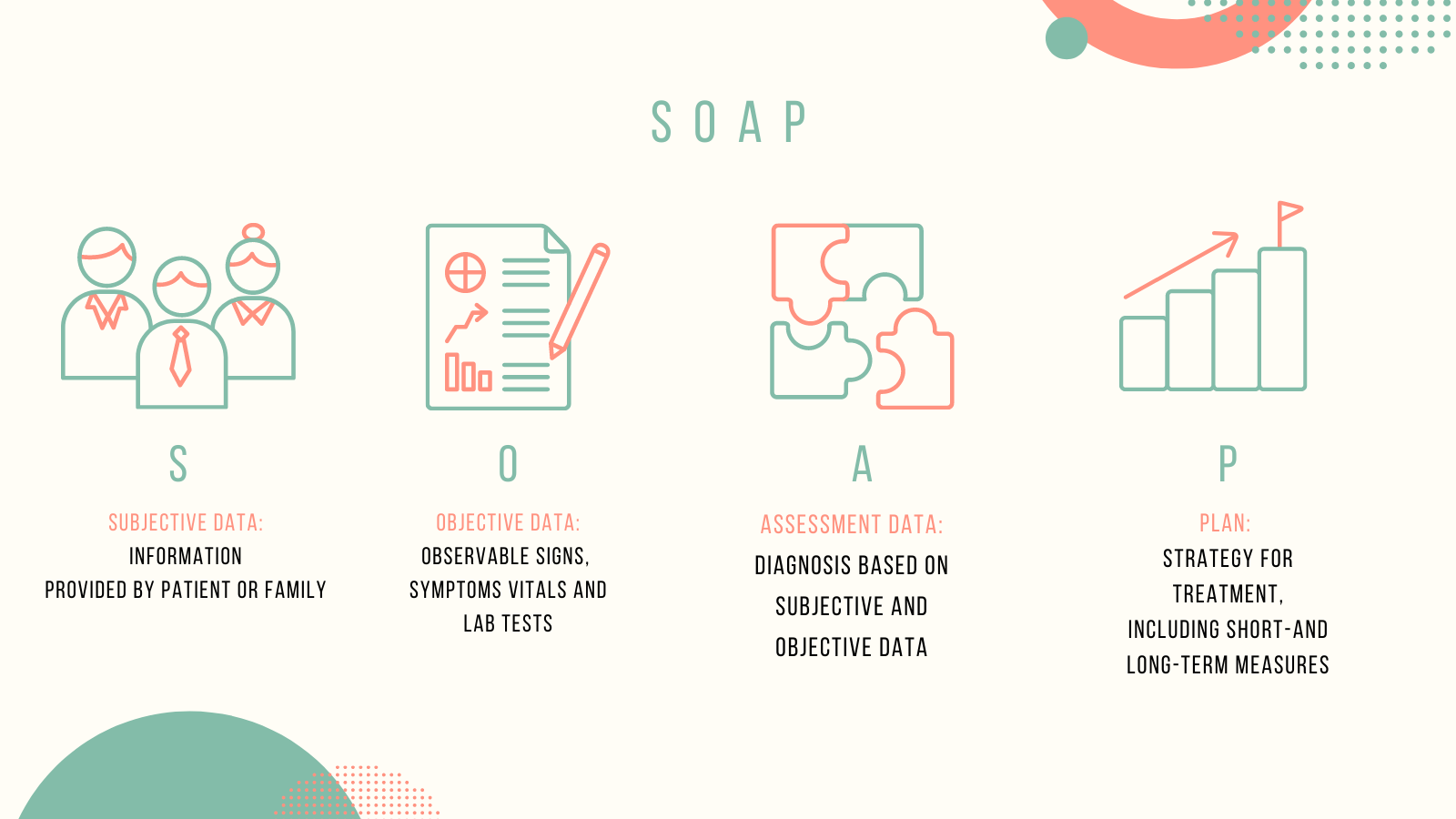
Although variations exist depending on the clinical setting or service line, the traditional SOAP note is broken into 4 sections:
- Subjective: This is a summary of what the patient, or the family depending on the situation, is telling you that day. In this section we are largely recording the patient’s impression of their situation, as told to the clinician, including the current status, characteristics and quality of their symptoms.
- Objective: This is where the clinician would note the most objective data or observations. Information here include items like blood pressure and heart rate, the results of the physician exam, and relevant results such as labs and radiology findings
- Assessment: The Assessment is a brief but total summary of the patient’s case including who they are, their relevant past medical history, the working diagnosis or diagnostic differential, and an update on the evolution of their condition or status since the beginning of the encounter period. This section, sometimes also called the “Impression”, is arguably among the most complex summarization tasks in clinical communication. It is remarkable and important because it requires the practitioner to synthesize sometimes vast information, on extraordinarily complex cases, into a concise, well written summary that does not exceed a few sentences. Within the SOAP note, this is the area we have focused on most at Pieces.
- Plan: The plan section usually involves an itemized summarization of the diagnostic or treatment plan, usually with the most acute or pressing issues first. The treatment plan usually includes the key tests we are waiting for and why, what remains to be deciphered, the treatment frequency, duration, procedures and the expected outcomes and goals.
If this structure is followed, the SOAP note allows clinicians to distinguish relationships between various problems, to properly account for and synthesize all the data, including the patient’s own subjective data; and – crucially–to pass on information to the next provider in the most effective and transparent fashion. It serves as a near-equivalent to a journalistic narrative (in terms of what has happened and the relevant circumstances), a scientific proof (in terms of how one has reached certain clinical conclusions), and a prediction set (in terms of the expectations, goals and predictions around what might happen under a certain diagnostic and treatment plan).
A well written SOAP note is a supremely effective communication method between doctors because it captures the totality of the thought process and reasoning behind a case. In the ideal process, the act of writing itself forces a practitioner to logically and systematically think through the patient’s situation in order to formulate an appropriate medical plan. We also know that the absence of effective communication contributes to serious causes of sentinel events, and factors into critical areas of health system improvement efforts such as readmissions, excess length of stay, and adverse clinical events.
At Pieces, we have been exploring how predictive modeling, natural language processing and natural language generation can help us contribute to an artificial rendition of the SOAP note, and perhaps provide a model for how AI systems may interact with clinicians. In my next post, we will dive into the Assessment section: If an AI is to replicate it, what must it be able to do?
Ruben Amarasingham, MD, is the founder and CEO of Pieces, Inc. He is a national expert in the design of AI products for healthcare and public health, and the use of innovative care models to reduce disparities, improve quality, and lower costs. Follow him on LinkedIn or Pieces to catch the next installation of this series.

